There is many things starting to STACK UP against the DEA/DOJ and their 5 decade war on drugs/pts. There is more and more practitioners – especially pharmacists – that are work with pharmacogenomics https://www.pharmaciststeve.com/21st-century-testing-to-help-chronic-pain-pts-justify-needing-higher-doses/ to help determine if a pt metabolizes different categories of medications differently. Pointing out that some pts are fast/ultrafast metabolizers of many meds are dealing with pts suffering from subjective diseases (pain, anxiety, depression, ADD/ADHD, various mental health issues) where historically there have been lab/test issues that have been ignored or dismissed they were involved in adversely affecting a pt’s QOL…
That the MME system has no science nor double blind clinical studies supporting their conclusions are nothing more than JUNK SCIENCE, but “they” have continued to use them as a ONE SIZE FITS ALL in the treatment of subjective diseases. https://www.acsh.org/news/2022/03/01/true-story-morphine-milligram-equivalents-mme-16154
“They” continue to blame Purdue Pharma was the genesis of the fabricate opioid crisis – yet it has been claimed that Purdue Pharma’s opioids were only 4% of all opioid Rxs.
“They” ignore that over the last decade, legal opioid Rxs have been reduced abt 50%, while concurrently the number of Opioid OD/poisoning have increased 7-8 fold, but only mention that those deaths were from Fentanyl – mostly failing to mention that the Fentanyl analog involved – that is mostly coming from China and Mexican cartels – is not the same FDA approved Fentanyl analog.
Now the 50 state AG’s sued the top 3 drug wholesalers and three largest chain pharmacies and besides getting these corporations to “cough up” tens of billions of dollars in fines for “contributing’ to the fabricated opioid crisis and at the same times getting these corporations agree to sell fewer control meds to pharmacies and chain pharmacies agreeing to dispense fewer controlled meds. Apparently doing so, in little regards for the pts valid medical needs for these medications. https://www.pharmaciststeve.com/dea-surrogates-are-trying-to-throttle-the-availability-of-controlled-meds-to-pts/
 Practitioners have been reducing or eliminating a pt’s pain medication and ignoring some predictable comorbidity complications, especially hypertensive blood pressure, heart attacks, strokes, increase pain, anxiety & depression & suicidal idealization.
Practitioners have been reducing or eliminating a pt’s pain medication and ignoring some predictable comorbidity complications, especially hypertensive blood pressure, heart attacks, strokes, increase pain, anxiety & depression & suicidal idealization.
Chronic Pain Detected in the Brain for the First Time
Real-world signals were seen mostly in the orbitofrontal cortex
https://www.medpagetoday.com/neurology/painmanagement/104635
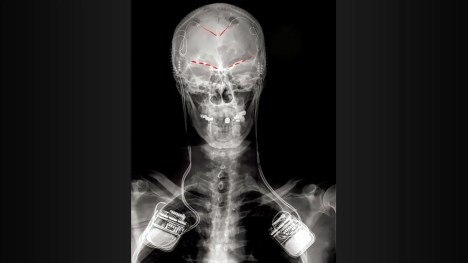
Chronic pain was detected in the human brain for the first time, researchers reported.
Data were collected over months from four participants with refractory neuropathic pain who had intracranial electrodes implanted, according to Prasad Shirvalkar, MD, PhD, of the University of California San Francisco, and co-authors. Over 3 to 6 months, participants reported their pain levels several times a day at home while the electrodes recorded their brain activity.
The recordings showed that chronic pain states were mostly associated with activity changes in the orbitofrontal cortex, Shirvalkar and colleagues wrote in Nature Neuroscienceopens in a new tab or window. This differed from transient or acute pain, which was associated with anterior cingulate cortex signals in two participants.
Functional MRIs have shown that the anterior cingulate cortex and orbitofrontal cortex regions are activated during acute pain experiments, Shirvalkar noted.
“We were interested to see whether these regions also played a role in how the brain processes chronic pain,” he said in a press briefing. “We were most interested in questions like how pain changes over time, and what brain signals might correspond to or predict high levels of chronic pain.”
Pain is one of the most fundamental experiences an organism can have, Shirvalkar observed. “Despite this, there is still so much we don’t understand about how pain works,” he pointed out. “By developing better tools to study and potentially affect pain responses in the brain, we hope to provide options to people living with chronic pain conditions.”
Chronic pain has no objective biomarkers to help guide diagnosis and treatment, Shirvalkar added.
In the U.S., the prevalence of chronic painis about 21%, affecting an estimated 51.6 million adults. New cases of chronic pain occur more frequently than new cases of diabetes, depression, or hypertension.
This study, which was supported by the NIH’s BRAINand HEAL initiatives, may be a first step toward developing novel methods for tracking and treating chronic pain, noted Walter Koroshetz, MD, director of the National Institute of Neurological Disorders and Stroke. “We are hopeful that building from these preliminary findings could lead to effective, non-addictive pain treatments,” Koroshetz said.
Shirvalkar and colleagues surgically implanted electrodes that targeted the anterior cingulate cortex and orbitofrontal cortex of four participants. Three participants had post-stroke pain and one had phantom limb pain.
Participants were asked to evaluate the pain they were experiencing — strength, type of pain, and how the pain made them feel — several times a day. They then clicked a remote-control device to create a 30-second brain recording of that moment.
Using machine learning methods, the researchers successfully predicted the pain severity scores of each individual from their orbitofrontal cortex activity with high sensitivity. Each person showed unique brain activity.
“Each patient’s biomarker was actually like a unique fingerprint,” Shirvalkar said. “I think that tells us something very important.”
In a separate analysis, Shirvalkar and colleagues examined how the anterior cingulate cortex and orbitofrontal cortex responded to acute thermal pain. In two participants, activity in the anterior cingulate cortex predicted acute pain responses.
The findings suggest that signals in the orbitofrontal cortex can track current chronic pain severity for neuropathic pain syndromes such as central post-stroke pain or phantom limb pain, the researchers said. The data also suggest that the brain may process chronic and acute pain differently in chronic pain patients.
“Global cerebral pain networks in all participants likely underwent rewiring over many years living with chronic pain,” Shirvalkar and co-authors wrote. “Still, ongoing ‘background’ chronic pain may have influenced acute pain perception even in the unaffected body side,” they noted.
Future work involving more participants may help determine whether different pain conditions share the orbitofrontal cortex activity found in these participants or how signatures may vary among persons with different pain conditions, the researchers added. Whether similar signals could be recorded non-invasively with electroencephalography (EEG) is not known.
Filed under: General Problems



















Great Thoughts Mary
What a wonderful breakthrough. What is happening with the states collecting vast amounts of money from the big pharma’s? We are victims of chronic intractable pain conditions that have been a casualty by Fed’s and State regulatory boards that have deceived the population by outright lying and deceit! There is not a short list of shrinks waiting to step in and collect on the billion of dollars collected
by the Feds and States. They have collected on our pain without suffering at all. They are collecting monies for the people that have chosen to use illegal drugs taking the chance it doesn’t kill them. They have been given choices while our choices have been taken away. Even drinkers and
smokers still have a choice to live or die.
Ted Cole
OMG,,, u don’t know,how much sense that makes to me,,gosh ,,that spot,,, i can feel some sorta effect,,,alllll the time there..Even when i take my pain medicine,,,that is amazing to me,,,Curious though,,is that not the same spot,,via imagery,,,they claim the ,”reward,” ,,but as a pain patient i claim thee relief center of the brain???????I thought I saw brain imagery 1 time,of methadone ,verses morphine,,and the morphine lit it up more/larger area then the methadone????Any who,,,im glad their finding the scientific proof of our forced physical pain,,,jmo,maryw